Akwaaba! Welcome to Ghana, the beautiful gold coast country which captured the hearts of millions worldwide during the recent Year of Return campaign. Ghana is a lower-middle income country (LMIC) located in West Africa, with a population of just over 30 million people and an ever expanding health innovation ecosystem.

Over the past few years, the number of health startups in Ghana has been growing at a rapid rate. Leading health startup mPharma is serving over 400,000 customers across five African countries, and has raised millions of US dollars in investment capital. While Redbird, launched in 2018, has expanded to serving 170+ pharmacies and over 20,000 customers with offices in both Accra and Kumasi. There is still significant room for growth, but it’s safe to say that Ghana’s social enterprises are successfully shifting to a larger focus on improving health and wellness.
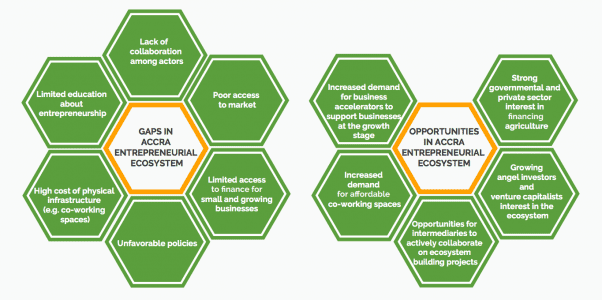
The Aspen Network for Development Entrepreneurs recently produced an Accra Ecosystem report, capturing major players, challenges, and opportunities within innovation and entrepreneurship throughout Ghana’s capital city. More than anything, this post represents Accra’s potential for entrepreneurial growth. While it cites challenges such as poor access to market, limited access to financing, and the high cost of physical infrastructure – it also recognizes the growing interest of angel investors/venture capitalists and increased demand for acceleration support, demonstrating a push towards further ecosystem support. For more details, please see the graphic below.
As entrepreneurship increases, Accra continues to face challenging health issues, paving the way for non-profit and for-profit startup initiatives to tackle issues ranging from emergency medicine to data interoperability. See below for a few key areas to watch in the coming years:
Emergency Medicine
Affordable, accessible emergency medical care is one the most pressing issues in Ghana. While the current government just procured over 250 new ambulances for the country (currently undergoing nationwide distribution), it does not currently utilize a centralized system for identifying patient locations, sending an ambulance for pickup, or determining the correct hospital for patient delivery. Due to a low number of trained specialists, and limited bed availability at many public facilities, patients can move from hospital-to-hospital in the back of an ambulance before ultimately reaching the location where they will receive care. While Zipline has recently entered the Ghanaian market, delivering blood and urgently needed medication via drones, many blood banks still sit empty – or are forced to remove donated blood from storage when it reaches its expiry date, but hasn’t yet been matched with an appropriate patient. A young woman facing postpartum hemorrhage may lose her life searching for a transfusion in her own blood type, while the same needed blood faces disposal across town.
Ghana is awaiting disruptive innovation in the field of emergency care, and investors should pay close attention to entrepreneurs who aim to solve this problem while actively engaging clinicians and emergency providers.
Mental Health
As with many African countries, Ghana maintains limited data regarding prevalence and treatment rates of mental health challenges for both youth and adults. Of patients who actively receive mental health care, the majority are treated at one of Ghana’s three psychiatric hospitals, five regional hospitals, or three teaching hospitals with small psychiatry units. While Ghana’s population is estimated to have reached 30 million people, it has approximately 18-25 trained psychiatrists actively in practice. The majority of ongoing care is provided by mental health nurses or community volunteers, with the highest trained professionals often stepping up to provide acute care. Private practice, outside the financial range of many Ghanaians, remains one of the only options for consistent, high-quality care. Even if care was readily available, cultural factors prevent many from actively pursuing it. A variety of factors such as family, religious, and professional expectations prevent people from seeking diagnosis or appropriate treatment.
While community advocacy campaigns (such as SmooothChat community discussions and PsychAidnLove’s Mental Health Meetups) have become commonplace in Accra, we see only a handful of interventions focused on providing accessible clinical care. One is MindIT, founded by Ghanaian medical student Atsu Latey, the USSD-enabled platform allows people to reach out via a feature phone short code to undergo an initial assessment and identify care providers in their area.
This area is ready and waiting for culturally-appropriate interventions and startups to introduce solutions, and we hope to see more emerge in 2020.
Emily Sheldon, AHIC
